NEONATOLOGY ON THE WEB

|
The Baby Incubators on the "Pike."
A Study of the Care of Premature Infants in Incubator
Hospitals Erected for Show Purposes.
Part 5.
By John Zahorsky, M.D.,
St. Louis, Mo.
St. Louis Courier of Medicine 32(4):203-219,
April, 1905.
(Continued from page 166, March, 1905, Number).
|
Additional Feeding.
For the infants taken out of the incubators additional feeding was
necessary; since ou supply of wet nurses was limited these babies had
to thrive on mixed feeding. During the service of my predecessor
certain proprietary foods had been given, for which he had been
criticised, probably unjustly so, since the basis of his feeding was
cows' milk. I determined at once to discontinue the use of
proprietary foods for reasons well known to pediatrists. Only cows'
milk, properly modified, was used. Walker-Gordon modifications were
rejected for the simple reason that these mixtures are twenty-four
hours old before delivery. Old milk can hardly be found satisfactory
with these feeble infants. Hence, I decided on a home modification of
the cleanest, freshest milk that could be obtained. Milk was finally
obtained from the Walker-Gordon Laboratory. The unchanged milk was
sent out to the Incubators by a special messenger. Milk that was
drawn the night before reached us about noon; it was, of course, kept
cold until delivered. It was allowed to stand on ice for three hours
and the lower half removed in the usual way. The top milk was used
diluted with whey made from the lower half. In other words, the
babies were fed on a whey and milk mixture, as has been advocated by
Rotch and Morse in this country, and Monti and others in Europe. The
mixtures were usually Pasteurized. Several times we had vomiting and
occasionally diarrhea from these mixtures, but in all cases it could
be referred to a high bacterial contamination of the milk. During the
hot months, especially in times of hot weather and low barometer, the
rapid change of milk is too well known to need especial study here.
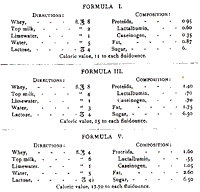
The following formulae give the directions for mixing and the
approximate composition of some of these mixtures. Subjoined is also
found the approximate calculated caloric value of the food, on which
the quantity of feeding was based. [See Figures]
It would be superfluous to give additional formulae. Altogether we
had nine such mixtures, but those given were used mostly. In
calculating the composition, the proteids are regarded in the
strength of 3.6 per cent, while the fat (one half of all the milk)
was computed as 7 per cent. In two mixtures (7 and 8) we employed top
milk containing one-third of the whole and which we calculated the
fat as 10 per cent in the mixture. The caloric value was calculated
from the ordinary rule that one gram of proteid or sugar yields 4.1
large calories, and that each gram of fat gives 9.3 calories.
In feeding these older babies we were again guided by the energy
quotient, which, of course, had to be controlled by the digestive
power of the infant. It is very difficult to maintain a constant
energy quotient when the change is made from human milk (calories, 21
to each ounce) to a milk mixture with only about one-half its caloric
strength. It was no wonder, therefore, that most infants lost in
weight when this change was made, even though the food was digested
perfectly.
While the whey and milk modifications were satisfactory as a food
for the older infants, especially when supplemented by one or two
breast feedings, it is difficult to understand how such a mixture
could be preferred to human milk. To give the infant a proper caloric
strength in such dilute foods necessitates the administration of
large quantities. I imagine it would be very hard to give a ten-days
old baby an energy quotient of 100 in a formula like No. 1.
V.
The Caloric Needs of the Premature Infant.
Heubner has laid down the rule that the food of the infant should
have an energy quotient of 100 calories. A quotient of energy which
is less than 70 calories is insufficient to sustain the needs of the
normal infant. Artificially-fed babies require an alimentation whose
energy quotient is 120 calories. Schlossman believes that a higher
energy quotient (110 calories) is necessary. [The energy quotient
signifies the number of calories in the food given to each kilogram
of the infant's weight.]
The subject is comprehensively discussed in an article by J. L.
Morse (American Journal Medical Sciences, March, 1904) to
which I must refer for more extended reference to the literature.
While it may be admitted that the figures of Heubner are rather
too high for large infants, for premature infants their value must
stand, since it is a well-known law that the small bodies lose
proportionately more heat than large ones. It has, therefore, been
assumed that premature infants require more calories per kilo than
those born at term. The cases of Beuthner and Schlossman leave the
matter still in doubt, although they found a higher energy quotient
necessary (113, 119). Morse from his interesting study also reaches
the conclusion that the caloric need of premature infants is
relatively greater than that of full-term infants.
A further corroboration of this need is found in the very
successful method of feeding adopted by Budin, who, calculating on
even a low basis of calories in human milk, uses an energy quotient
of 120 to 130 calories in alimentation.
I offer this additional evidence of the caloric needs of the
premature infant. While I recognize that, as the milk of wet nurses
was not analyzed quantitatively, and an average composition was
assumed, these figures are by no means absolutely correct. Yet, it is
the method usually adopted to calculate the caloric needs. Morse is
certainly rather severe in criticising results based on this
estimate, when he states that figures based on such an average
caloric value per liter of milk can not be of great value. It would
be an almost impossible task to analyze each separate food supply of
the infant, since it is known that the milk varies in composition on
different days and even on different periods of the day. Then it
would make a marked difference whether the infant obtained its milk
when the breast was overfilled or nearly empty. It will be seen,
therefore, that nearly all calculations in regard to the need of the
energy quotient when human milk is used must be based on an average
caloric value.
We had five wet nurses who furnished the milk, and their milk was
emptied into a bottle whence it was fed to the babies. It was often
mixed, that is to say, one baby would receive milk from more than one
wet nurse on the same day. I feel, therefore, that we are perfectly
justified in using an average composition in making calculations.
Then, again, the present purpose is not so much to establish a
maximum or minimum line, but to find a practical average which can be
used by physicians in the feeding of premature infants. The rule has
already been given in the previous section, it remains now to study
the individual cases and see if the proper needs have been formulated
in the rules for feeding.
It took some little time after I took charge to get the daily
weights and quantities sufficiently exact, so that the figures given
are the results after September 18th.
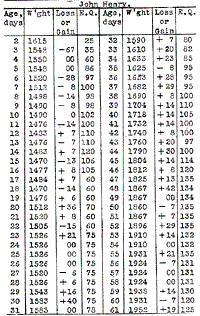
In analyzing the record of the food and weight of John Henry
(Table 16) several interesting facts may be noticed. In the first
place, trying to increase the milk in the first two weeks as rapidly
as Budin directs, a severe attack of indigestion was induced. On the
fourteenth day with the alimentation having an energy quotient of 120
calories, about what his rule of feeding would give, our patient had
frequent green stools showing undigested food. Moreover, he had
several attacks of cyanosis and subnormal temperature. On the
seventeenth day the food had to be decreased and an additional supply
of water given. The dyspeptic symptoms disappeared in about ten days,
and he began to have a good daily gain on a quotient energy of about
75 calories. It will be observed that during the ten days (27th to
37th day of life) he gained 162 grams, or an average of 16 grams a
day. This record rather supports the assertion of Czerny and Keller
(Des Kinder Ernahrung, page 385) that some infants gain 15
grams daily on an energy quotient of 70 calories. During another
period (46th to 56th day of life), with an energy quotient of 130
calories, he gained only 112 grams, or an average of 11 grams daily.
Of course, the first period was immediately after a period of
indigestion and loss in weight; the gain may be probably accounted
for by a storing of water. Another period when the quotient energy
was near 100 calories (35th to 45th day) gave a daily gain of 18
grams. A much higher quotient energy gave no higher gain. Even later,
when on account of supplying his hunger, or putting him to the breast
he took a still larger quantity of milk his gain was no greater.
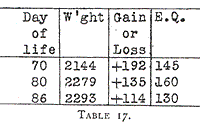
Table 17 gives a brief resumé of his subsequent history.
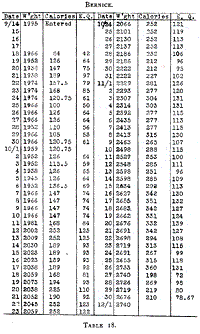
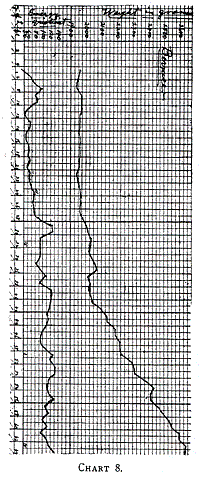
In the case of Bernice (Table 18, Chart 8) I feel sure that our
method of feeding was rather too cautious at the beginning. In her
case the method of feeding based on the energy quotient had not as
yet been adopted. Notice the sharp rise in weight on September 22nd,
when the energy quotient on the previous day was near 100 calories.
She certainly corroborated the view of Heubner that an infant can not
gain on an energy quotient of 70 calories or less. The first good
gains are reached when the energy quotient is over 80 calories.
During the period of October 11th to 21st (energy quotient near 90
calories) she gained an average of 6 grams daily. During the period
of October 22nd to November 1st, with an energy quotient of about 110
calories, she gained 8 grams daily. On the following period of ten
days the average gain was 29 grams daily, with an energy quotient of
nearly 115 calories.
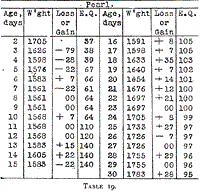
In the case of Pearl (Table 19) the alimentation had to be reduced
on the fifteenth day as dyspeptic symptoms appeared. From the
fifteenth to the twenty-fifth day with an energy quotient near 100
calories the average daily gain was about 15 grams. Following this
period the food quality was relatively less and the gain in weight
was correspondingly less.
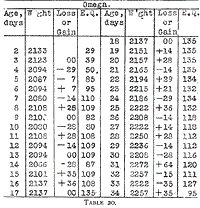
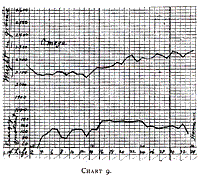
Omega (Table 20 - Chart 9) was a large baby and we should expect a
larger gain on the same energy quotient, but as a matter of fact we
find no great difference. The first period of ten days (15th to 25th
day) with an energy quotient of 10 to 130 calories the average daily
gain was only about 15 grams. On the following ten days, with a
lessened food supply, the gain was about 4 grams daily. This was
caused also by slight indigestion superinduced by excessive feeding
(17th to 24th day). It only emphasizes the fact that it is dangerous
to give an alimentation that exceeds an energy quotient of 120
calories during the first few weeks.
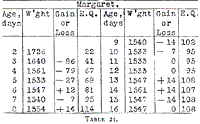
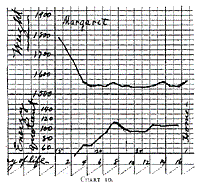
The rapid increase in the food in the case of Margaret (Table 21)
did not succeed in producing a rapid gain. Time must always be
allowed for the weak digestive apparatus to adapt itself even to
mother's milk. She did not stay with us long enough to determine
digestive power as the Institute closed and she was sent home in good
condition.
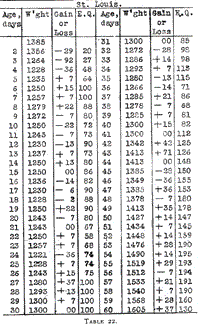
The history of St. Louis (Table 22) is exceedingly instructive. By
the rapid increase of the food to an energy quotient of 100 calories
on the sixth day the initial loss in weight was checked, but an
indigestion followed which was treated by a reduction in food, and
for twenty days there was no gain in weight. On the twenty-seventh
day there was a great improvement in stools and the food was
increased to an energy quotient of 100 calories. But pushing the food
beyond that again brought on greenish stools. On the forty-first day
the infant had not yet regained its original weight, and the stools
having improved a forced alimentation was tried, gavage being used at
times. Mother's milk was given in increasing quantities so that its
energy quotient on the fifty-fourth day reached 195 calories.
Probably this was overfeeding -- yet the infant gradually became
accustomed to this food and on the following twelve days (48th to
60th day) gained on an average of 19 grams daily. On the following
ten days (not shown in the table) he gained 10 grams daily on an
energy quotient of 130 calories. His history will be more
specifically discussed under "Indigestion."
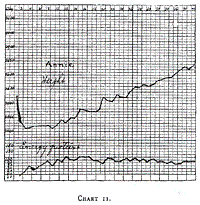
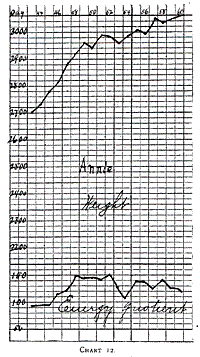
Annie (Chart 11) illustrates the gradual increase of food, and how
the loss in weight is checked when an energy quotient of 70 calories
is reached. She gained nicely on an alimentation having an energy
quotient of 95 to 100 calories. Chart 12 shows how a larger increase
of food does not increase the gain in weight but slightly. An energy
quotient of 150 calories was too large. She gained very rapidly (30
grams daily) on a food having an energy quotient of 120 to 130
calories (58th to 64th day). She was a large baby to begin with and
her growth was uninterrupted.
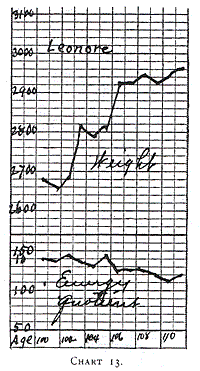
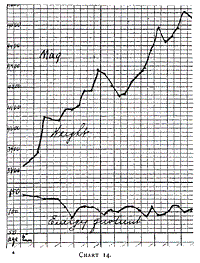
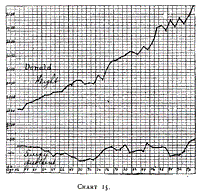
Charts 13, 14 and 15 (Leonora, Mag. and Donald) illustrate the
growth on mixed feeding. These were graduates, and the curves show
their food and weight during certain periods of their life. Again, we
notice that an energy quotient of about 120 to 130 calories is most
satisfactory. Higher quantities give rise to indigestion. When the
energy quotient is the same, and digestion is perfect it is
impossible to draw any distinction between modified cows' milk and
human milk in these older babies.
Deductions.
1. The use of the energy quotient as a basis of infant feeding is
entirely practicable.
2. An energy quotient of 70 calories should be considered the
minimum for maintaining the metabolic equilibrium. In many cases a
steady growth may be obtained on this alimentation.
3. Most premature infants require human milk having an energy
quotient of 100 to 120 calories in order to insure a steady gain in
weight.
4. Quantities of human milk having an energy quotient of more than
135 calories should only exceptionally be given, as this favors
indigestion and subsequent loss in weight.
5. In older infants there is little difference in growth when
human or bovine milk is used, provided the digestion is perfect and
the energy quotient the same.
Figures
|
|
Formulas I, III, and V.
|
|
|
Table 16.
|
|
|
Table 17.
|
|
|
Table 18.
|
|
|
Chart 8.
|
|
|
Table 19.
|
|
|
Table 20.
|
|
|
Chart 9.
|
|
|
Table 21.
|
|
|
Chart 10.
|
|
|
Table 22.
|
|
|
Chart 11.
|
|
|
Chart 12.
|
|
|
Chart 13.
|
|
|
Chart 14.
|
|
|
Chart 15.
|
(To be Continued.)
Return to the Contents Page
Created 6/17/2000 / Last modified 7/16/2020
Copyright © 2000-2020 Neonatology on the Web / webmaster@neonatology.net
















